MAKING SENSE OF OMEGA-3: The Skinny on Fatty Acids, Fish Oils and Brain Health
 Personally, I take a lot of nutritional supplements, but it is difficult to know which of these is really necessary. When patients ask what they ought to be taking I can only answer confidently that only Essential Fatty Acids (EFAs, Fish Oil) and possibly Vitamin D seem to be necessary for the typical well-nourished American, methyl-folate may be needed for people on anti-depressant drugs, and B12 sublingual may be important for older people and non-meat eaters. Plus, Resveratrol looks very promising,
Personally, I take a lot of nutritional supplements, but it is difficult to know which of these is really necessary. When patients ask what they ought to be taking I can only answer confidently that only Essential Fatty Acids (EFAs, Fish Oil) and possibly Vitamin D seem to be necessary for the typical well-nourished American, methyl-folate may be needed for people on anti-depressant drugs, and B12 sublingual may be important for older people and non-meat eaters. Plus, Resveratrol looks very promising,
In this communication, I will focus mainly on the all-important Essential Fatty Acids, and particularly on Fish Oil, an Omega-3 poly-unsaturated fatty acid, known as Eicosapentaenoic Acid (EPA). EFAs are well-established contributors to cardio-vascular health and protectors against sudden cardiac death. Here, I will focus on EFAs and brain health. And mental health.
Note, a new study from UCLA announced today has demonstrated that the level of Omega-3 DHA in red blood cells indeed correlates with brain volume and memory in older men and women–see below.
The Journal of Clinical Psychiatry recently devoted two articles and a Commentary on Fish Oils for depression, under a weighty cover headline: Eicosapentaenoic Acid for Depression: A Meta-analysis of Clinical Trials (Vol 72, December 2011, Num 12). In short, there is clear evidence that Fish Oils can treat depression and some evidence that low levels of Omega-3s are associated with a suicidal outcome. Last September, at the ISNR 19th Annual Conference in Phoenix, Daniel Johnston MD, MPH, who is Medical Director of the Pentagon’s Comprehensive Soldier Fitness Program, gave a beautiful review of EFAs and their importance in brain fitness. Most of the information in this post derives from my notes of that lecture as well as the slide delineating Fatty Acid Families.
With that as a start, I’d like to help you make some sense of this highly important topic.
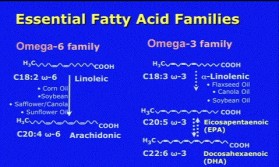 One crucial point is that the typical American diet, even one high in poly-unsaturated fatty acids, is at risk of being relatively deficient in Essential Fatty Acids. The problem is that our diets are loaded with Omega-6 fatty acids from grain sources like corn, soybean, safflower, and canola oils—which directly compete with the good Omega-3s. Omega-6 fatty acids are converted to Arachnodenritic Acid (ADA), which promotes an inflammatory response in blood vessels.
One crucial point is that the typical American diet, even one high in poly-unsaturated fatty acids, is at risk of being relatively deficient in Essential Fatty Acids. The problem is that our diets are loaded with Omega-6 fatty acids from grain sources like corn, soybean, safflower, and canola oils—which directly compete with the good Omega-3s. Omega-6 fatty acids are converted to Arachnodenritic Acid (ADA), which promotes an inflammatory response in blood vessels.
The ratio of Omega-3s to Omega-6s is important. The average American has about 4% Omega-3s; the average Japanese has about 8%. Epidemiological studies indicate that Japanese on traditional diets have significantly less cardiovascular disease and sudden cardiac death than Americans.
Omega-3 predominantly comes from fish oils and is interconverted between Eicosapentaenoic Acid (EPA) and Docoshexaenoic Acid (DHA) . The ratio of these two Omega-3s is probably also important. The meta-analysis in the Journal of Clinical Psychiatry clearly indicated that for depression, omega-3 supplementation is most effective in a 60%/40% mixture of EPA/DHA with a ceiling at around 2,000 mg/d of EPA in excess of DHA.
Although Omega-3 also comes from alpha-linoleic acid in flaxseed, canola, and soybeans, contrary to frequent assertions, it is doubtful that these grain sources can balance the Omega-6 (linoleic acid) also contained in the same grains. The addition of monosaturated fats (Omega-3s and Omega-6s are known as poly-unsaturated Fatty Acids), may be helpful. Note that as the following chart shows, some vegetable oil sources of monosaturated fats will also contain inflammatory-stimulating Omega-6 fats.
Approx 40 % of the fatty acids on the orbitofrontal cortex are highly unsaturated omega-6 and omega-3 fatty acids. 1/3 of these are DHA. A 2007 study published in the medical journal Lancet demonstrated that women who consumed more seafood when pregnant had smarter babies. And this has been corroborated in many subsequent studies. The American Academy of Pediatrics recommends supplementation of EFAs during pregnancy and lactation.
Studies have shown cognitive benefits of Omega-3 in healthy subjects:
- Improved mood profile
- Increased vigor
- Reduced anger
- Reduced anxiety
- Improved reaction time
- Improved sleep efficiency and improved cognitive function after sleep deprivation (mitigates sleep loss effects).
Dementia: Astoundingly, a 2006 study published in the Archives of Neurology intake of an average of only 180 mg/day of DHA was associated with a significant 47% reduction in the risk of developing all-cause dementia.
Depression. How do EFA’s help? Here is a list:
- They alter neuronal fluidity by displacing cholesterol from neural membranes;
- Influence the function of membrane receptors, modifying dopaminergic and serotonergic neurotransmission;
- They decrease monoamine-oxidase B activity;
- Regulate membrane-bound enzymes (Na/K-dependent ATPase) which decreases energy consumption requirements in the brain;
- Modulate glucose uptake;
- Increase dendritic arborization (outgrowth) and synapse formation, decrease neuronal apoptosis;
- They compete with Arachnodenritic Acid (the product of Omega-6s, see above) for enzymatic action generating an anti-inflammatory response;
- Lower plasma DHA at baseline predicts greater risk of future suicide attempts;
- Controlled double-blind pilot study in childhood depression: 600 mg EFAs, ages 8-12.5. Depression rating scales significantly improved in treatment vs placebo;
- Deliberate self-harm 50 % reduction in depression, 35 % reduction in suicidal thinking; 33% reduction in perception of stress; 30% improvement in “happiness”.
Teacher-rated ADHD symptoms (blind): substantial changes in every measure including also Social Problems, Perfectionism, and Opposition.
Recommendations
Everyone’s diet should include Omega-3 Essential Fatty Acid supplements. Fish Oils are better than vegetable sources because of the inflammatory effects of Omega-6s. Fancy products like krill oil are unnecessary and may lead to depletion of this important ocean resource. A study of few years ago in Consumer Reports demonstrated that all products on the market were free of toxic substances. It is important that Fish Oils be relatively fresh and not oxidized. 3-4 grams daily seems best for cognitive /memory performance and mood/behavior/focus issues; for genera health (brain and heart) 2-4 gm/day.
The ratio of Omega-3s to overall fatty acids can be easily measured with the Omega-3 Index: a measure of the amt of EPA +DHA in red blood cell membranes expressed as the percent of total fatty acids. There are 64 fatty acids in this model membrane, 3 of which are EPA or DHA. The correlation between Executive Function of the Omega-3 Index has been established. The procedure is a simple finger stick to produce a drop of blood which is placed on blotter paper and mailed to the lab. Omega-3 in red blood cell tissue reflects levels of omega-3 fatty acids in the brain.
I offer the Omega-3 Index in my office at no markup. The lab currently charges me $90 for each test and the patient is billed $90. I also offer Essential Fatty Acids at wholesale cost from the Life Extension Foundation, and pass that exact cost on to the patient (because there is no profit, it is also exempt from California sales tax).
Note, a new study from UCLA announced today has demonstrated that the level of Omega-3 DHA in red blood cells indeed correlates with brain volume and memory in older men and women.
The February 28, 2012 edition of the journal Neurology® reports a beneficial effect for higher red blood cell membrane levels of docosahexaenoic acid (DHA, an omega 3 fatty acid) on brain volume and memory in older men and women. “To our knowledge, no prior study has related red blood cell fatty acid composition to subclinical markers of future dementia,” the authors note in their introduction to the article.
For their research, Zaldy S. Tan, MD, MPH, of the Easton Center for Alzheimer’s Disease Research and the Division of Geriatrics at the University of California at Los Angeles and colleagues measured red blood cell omega-3 fatty acid levels in 1,575 dementia-free subjects with an average age of 67. Magnetic resonance imaging (MRI) assessed brain volume, and cognitive tests evaluated various aspects of memory and mental function.
Dr Tan’s team found a reduction in total cerebral brain volume, visual memory, executive function (which includes organizing and multi-tasking) and abstract thinking, among those whose DHA intake was among the lowest 25 percent of participants compared to those whose intake was higher. “People with lower blood levels of omega-3 fatty acids had lower brain volumes that were equivalent to about two years of structural brain aging,” Dr Tan observed.
Participants in the lowest 25 percent of DHA also had greater white matter intensity volume, which is increased in small vessel disease and has been associated with an increased risk of stroke and dementia. The authors remark that DHA lowers blood pressure, reduces the risk of clots and decreases serum triglyceride levels, all of which benefit the vascular system and may help delay the onset of brain aging.
“Lower red blood cell DHA levels are associated with smaller brain volumes and a ‘vascular’ pattern of cognitive impairment even in persons free of clinical dementia,” the authors conclude. “The association between lower red blood cell omega-3 fatty acid levels and markers of accelerated cognitive and structural brain aging observed here should be confirmed in other populations and extended in the future to include dementia outcomes.” This news courtesy of Life Extension Bulletin, 2/28/12.
Further Reading: The Omega-3 Connection by Andrew Stoll MD may be the most useful book currently available. It was published in 2002. In August 2012, William Sears MD will bring out The Omega-3 Effect.

